


Behind every bag of donated blood is a long process about safety, timing, and trust. From trauma care to cancer treatment to childbirth, donated blood makes countless procedures possible. But even to date, transfusions are not completely risk-free.
That is why pathogen inactivation is now a big subject and why Cerus has built a business around one question: “What if, instead of trying to detect every possible infection in donated blood, you made the blood safer by default?”
Blood screening has come a long way and is far safer than it was decades ago, thanks to donor screening and laboratory testing, but the problem remains. New tests detect known viruses before the blood is used in a patient, but “most” does not mean “all.”
Some are undetectable at low levels. Furthermore, testing standards vary around the world, and there is an imbalance in safety measures. Even at the top healthcare institutions, there is always an open window where viruses are present but invisible.
While the problem remains unsolved, hospitals still demand blood at a high rate. Trauma cases, cancer treatments, elderly patients, surgeries, and so on all require a blood supply. They cannot wait for the blood to be in “perfect condition.” This demand makes proper testing impossible.
These conditions explain why blood safety innovation is moving from detection toward prevention. Pathogen inactivation is simple: rather than looking for every virus or bacteria in donated blood, it neutralizes them before use.
Hospitals and blood banks cannot work with complicated workflows. To solve this issue, Cerus Corporation was founded by Dr. Laurence Corash, B.J. Cassin, and Stephen. T. Issac created a system that could fit into blood bank workflows. The process uses a photochemical process that combines a specialized compound with ultraviolet light. When added to plasma or platelets, the compound binds to nucleic acids. And after the exposure to ultraviolet light, it binds to and disables the genetic material inside pathogens and residual white blood cells.
This treatment does not affect the functional properties of blood needed for transfusion. Platelets still clot. Plasma still carries essential proteins. The aim is not to make blood sterile but to make it safe. The only thing that changes is the risk profile and the fact that the treated blood components can no longer transmit infection.
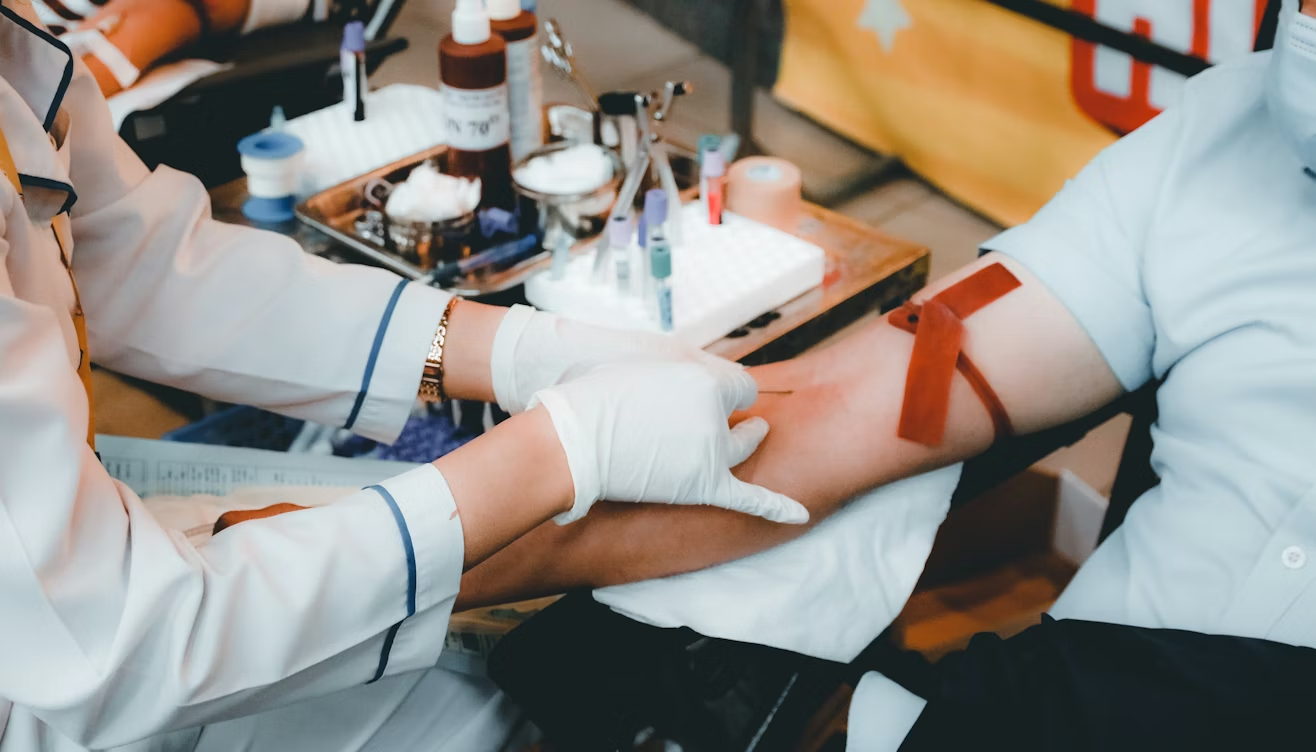
Image: Unsplash
Tests played a major role in the routine blood safety measures. The donated blood is tested for common pathogens such as HIV, hepatitis B, and hepatitis C. This approach saved many lives, but imitations became obvious when new viruses entered the picture.
Testing assumes you are already aware of potential threats. However, outbreaks do not have a predictable pattern. New viruses appear out of nowhere, and some take time to be properly understood or even screened after potential damage has occurred.
Pathogen inactivation changes that equation. It was capable of detecting both known and unknown pathogens, even the suspected ones and the ones that were ignored. The risk levels associated with bacterial contamination, which remains a concern for platelets in particular, were also lowered.
What this means for blood transfusion testing is that there will be fewer blind spots and improved ways to detect hidden pathogens.
Some countries, like Japan, the USA, and Germany, among others, have advanced screening procedures. While some other countries, primarily located in Sub-Saharan Africa and South Asia, are struggling with limited resources, trained experts, or equipment.
In these struggling countries, what solution can be made available for them? Pathogen inactivation is a way to improve safety without a complex testing infrastructure. This makes it essential for regions that are high on the risk scale because of a lack of adequate testing equipment.
This is one of the many reasons why Cerus’ blood safety technology has been accepted globally. It has a standardized layer of protection and is capable of working in any kind of environment, not just ideal ones. Cerus’ systems are already used in several countries, like France, Switzerland, and Spain, amongst others, showing that there is a growing recognition that blood safety needs solutions to protect everyone.
The blood pathogen inactivation system undergoes extensive clinical testing to obtain data indicating how treated plasma and platelets are expected to perform in real patients. Also, before it is approved, it must be proven that it is not harmful to patients or will not jeopardize blood transfusions. The regulatory approvals the procedure has received in multiple regions demonstrate their confidence in its safety and effectiveness.
Still, these systems need each other to work. They were not built to stand alone. Blood screening, donor selection, and testing remain important. Pathogen inactivation adds an extra layer of safety rather than replacing existing safeguards. Modern blood safety is based on several overlapping safeguards that work together.
Blood supply chains are weak. They depend on donors, transportation, storage, timing, and transfusion under strict conditions. Any little inconvenience can slow things down.
Cerus systems were designed to seamlessly integrate into the existing workflow, and this makes blood transfusion a lot safer with minimal disruption. It also offers more confidence during shortages, simpler inventory management, and being equipped to handle outbreaks or emergencies.
During public health emergencies, when unknown pathogens may emerge rapidly, having pretreated blood available adds resilience to healthcare systems.
Cerus sits at the point where biotechnology and healthcare infrastructure meet. It is not interested in coming up with new methods of blood transfusions but in strengthening the systems that nearly every other treatment depends on.
Surgeries, cancer care, trauma care, emergency medicine, and chronic disease treatment all depend on safe blood. Improving the processes involved in it improves everything else as well, and that is what Cerus represents.
As healthcare systems gear up for future challenges, blood transfusion will remain a foundational safety concern. Blood transfusions will most likely never be risk-free. But the goal is to reduce the risks as much as possible by neutralizing pathogens before transfusion.
Pathogen inactivation will continue to play a major role as part of a multi-layered safety strategy by detecting the risks that exist and designing around them. And over time, this approach is likely to become a standard routine. In doing so, Cerus supports a healthcare reality where safety isn’t just tested for but built in. As a testament to its contribution, roughly 20 million transfusable doses have been approved for patients.
Wrapping up, Cerus exists because blood transfusions are never completely risk-free, and the system cannot depend on mere hope. Pathogen inactivation provides a way to make sure the patients are safe by design and not just detection. Prioritizing infection prevention, resilience, and patient safety is quickly turning blood safety technologies into infrastructure rather than optional upgrades. And as healthcare systems continue to grow, technologies that make blood transfusion processes safer may yet become some of the most important innovations in supporting the broad spectrum of physical and emotional vitality. By prioritizing safety, Cerus ensures the purity and vitality of the body are maintained during critical medical procedures.